Need Help ?
(727)888-6759
A revenue-guaranteed AR management platform that operates the way you do
Medcubics AR Management was designed by professional medical billers to provide you with the automation you need to manage a successful business. Whether you’re a medical billing manager in a physician’s office or a medical billing company owner seeking higher returns on accounts receivables, AR Management is an intuitive AR program that will work the way you work by reliably delivering payments and preventing billing errors.
The tools in AR Management provide you with detailed reports on denied claims and give you a snapshot of all outstanding claims with patient details, so you never miss a rogue bill.
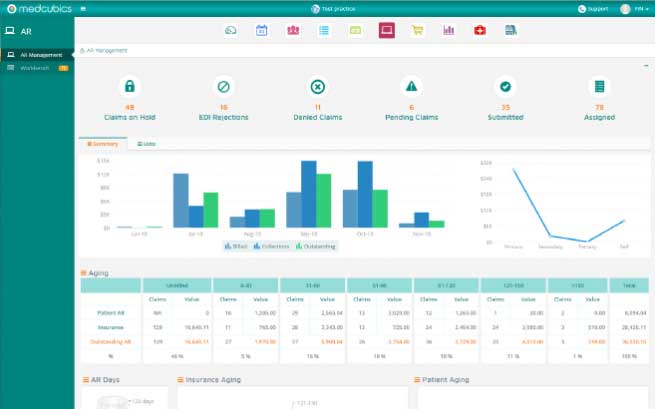
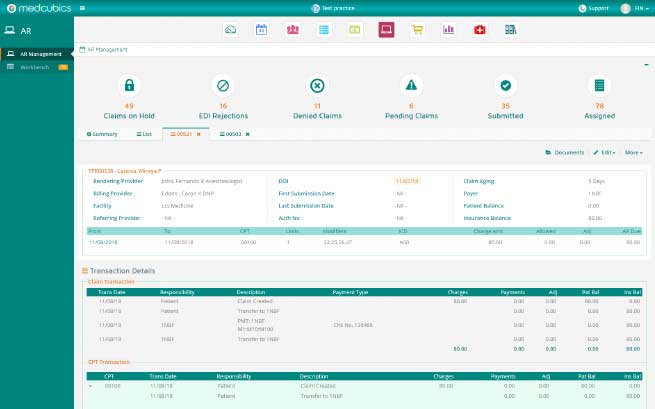
Medcubics creates claim processing reports and tracks rejected or denied claims that need to be corrected and resubmitted automatically. It also includes comprehensive reporting and workflow capabilities that allow you to evaluate upaid claims by status and age, allowing you to prioritise collection efforts to maximise cash flow.
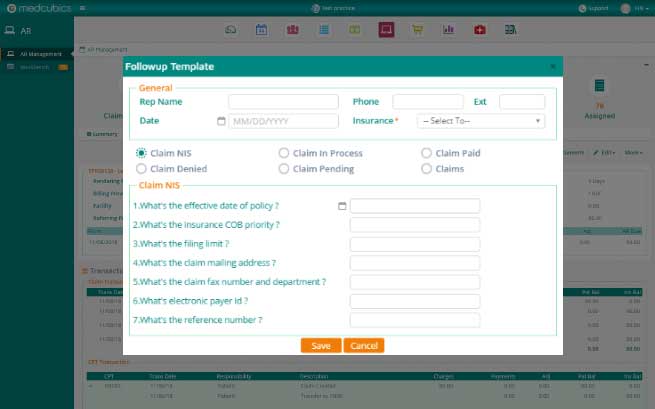
For any claim scenario, insurance follow-up templates are easily available for AR staffs, assisting them in probing the correct questions that lead to claim settlement. Claims are automatically evaluated and categorised by age and status, and are grouped by categories for insurance, patient, and workers compensation.
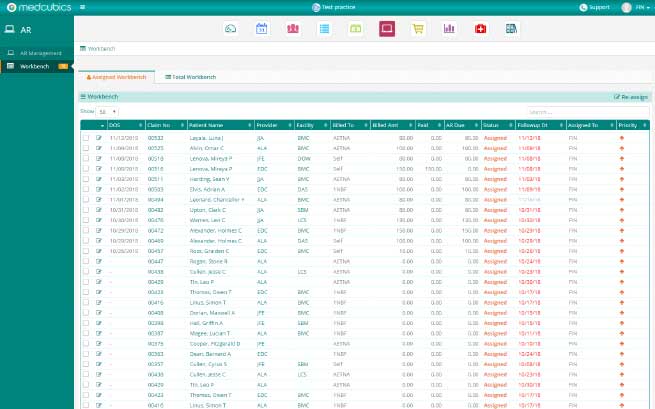
You may use AR Management to create rules that divide labour into activities inside the billing office and organise your daily workflow by role. As you and your colleague set up activities according to AR Management's user-friendly protoco, you'll reduce misunderstanding and improve workflow efficiency.
Simply dig down into the relevant insurance claims to correct and resubmit the claims with or without supporting documentation – electronic/fax/print. Appeals are prepared and submitted using pre-programmed templates. Insurance payments, adjustments, and future follow-up are all done through our AR interface.
Our Benefits
- Assists in prioritization of AR information according to financial risk
- Our AR workbench engine helps allocate claims to users based on prioritization
- Resolve Denials and Rejections Efficiently
- Optimizes revenue capture and decreases days in AR
Experience medcubics via live demo
Schedule a personalized demo, guided by a live expert

